A reduction in pressure while ascending at the end of a dive will release dissolved gas (principally nitrogen) from solution in the tissues and blood and consequently form bubbles in the body.
A reduction in pressure while ascending at the end of a dive will release dissolved gas (principally nitrogen) from solution in the tissues and blood and consequently form bubbles in the body.
DCI results from the effects of these bubbles on organ systems. The bubbles may disrupt cells and cause loss of function. They may act as emboli and block circulation especially in the capillaries. They may cause mechanical compression and stretching of the blood vessels and nerves.
Additionally, the blood-bubble interface acts as a foreign surface, activating the early phases of blood coagulation and the release of substances from the cells lining the blood vessels causing vasoconstriction which can worsen the effects of a blocked vessel. If not managed properly the blood bubble interface promotes an inflammatory reaction that may lead to permanent damage.
Most DCI comes on in the first few hours after the end of a dive. Some starts before leaving the water. Most cases have developed symptoms within 24 hours. Curiously it may take an affected diver 6 – 8 days or more to recognize the symptoms and seek advice and treatment.
DCI is divided into 2 categories. Type I was mild and described pain only, bends and skin bends. Type II included everything else. Now it still seems useful to use the old names but since the lines between Type I and Type II are blurred by considerable overlap, the classification is not so useful and a description of the symptoms, their speed of onset and their rate of progress are of more use to rescue authorities and to hyperbaric physicians and chamber operators. All DCI should be treated as serious even though the actual symptoms may appear mild. DCI can now be thought of as having 3 categories:
-
- Type I Typically pain in a joint or joints. Can be very painful or just niggly (hence niggles). This is uncommon in sport divers unless dives have been long. Do not ignore other symptoms such as extreme tiredness or loss of sensation placing this sort of bend in a more serious category. Resist the temptation to describe it as a mild bend.
-
- Type II (serious) All symptoms in this category should be regarded as serious even though they seem mild. They should all be treated. A full description of the range of symptoms appears below.
- Pulmonary Barotrauma and Arterial gas embolisation (AGE).
TYPE 1 DCI
Type I DCI is characterised by:
-
- Mild pains that begin to resolve within 10 minutes of onset (niggles)
-
- Pain in a joint or joints with the consequent loss of function of the joint is the classical bend named in parody of the fashionable Grecian Walk of the late 19th Century It occurs in up to 70-85% of patients with DCI.
The pain is often described as a dull, deep, throbbing, toothache-type pain, usually in a joint or tendon area but also in tissue. The shoulder is the most commonly affected joint in divers after a shallower than 40 metre dive, whereas the knees are affected more in deep divers. The pain is initially mild and slowly becomes more intense. Because of this, many divers attribute early DCI symptoms to overexertion or a pulled muscle.
Upper limbs are affected about 3 times as often as lower limbs. The pain of Type I DCI may mask neurological signs that are hallmarks of the more serious Type II DCI.
Skin bends, rashes, mottling, itching and lymphatic swelling have frequently been included in the Type I canon, However modern experience suggests that they are serious symptoms in their own right and should always be investigated and treated. They are described here for convenience.
-
- “Skin bends” that cause itching or burning sensations of the skin; or
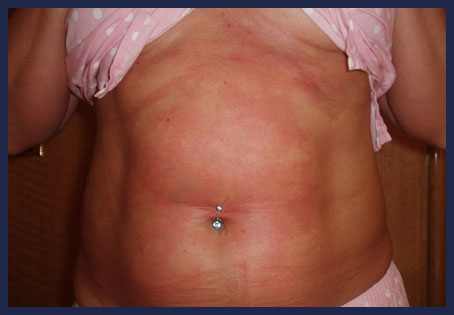
Skin rash, which generally is a mottled rash causing marbling of the skin or a violet coloured rash which is most often seen on the chest and shoulders. On rare occasions, skin has an orange peel appearance.
It is important that this is not confused with other causes of a rash whilst diving. A suit squeeze will generally have a different pattern and look more like bruising, whilst a neoprene contact dermatitis will be in areas where a suit rubs, such as the neck or cuffs.
Read the article on Skin Bends
-
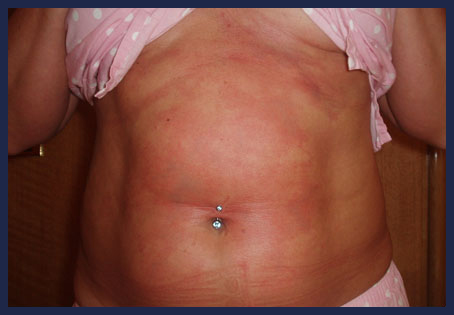
- Lymphatic involvement is uncommon and usually is signaled by painless pitting oedema. This usually starts on the chest and will tend to move down the trunk over the next few days, finishing in the lower legs. At any stage if the thumb is pressed into the swelling for 15 -30 seconds it will leave an impression. The mildest cases involve the skin or the lymphatics.
- Some authorities consider anorexia and excessive fatigue after a dive as manifestations of Type I DCI. We see them as serious symptoms requiring investigation.
TYPE II DCI
Type II DCI is characterised by nervous system involvement pulmonary, lung symptoms and circulatory problems such as hypovolaemic shock. Pain is reported in only about 30% of cases. Because of the anatomical complexity of the central and peripheral nervous systems, signs and symptoms are variable and diverse. Symptom onset is usually immediate but may be delayed as long as 36 hours.
NERVOUS SYSTEM
The spinal cord is the most common site for Type II DCI; symptoms mimic spinal cord trauma. Symptoms such as lower back pain may start within a few minutes to several hours after the dive and may progress to paresis, paralysis, paraesthesiae, loss of sphincter control. Girdle pain around the upper abdomen or the lower trunk is a common first symptom while higher up the cord, neck and arm symptoms may predominate. This form of DCI can be progressive and dynamic and does not follow typical peripheral nerve distribution patterns. This strange shifting of symptoms confuses the diagnosis, differentiating DCI from traumatic nerve injuries.
Other common symptoms include headaches or visual disturbances, dizziness, tunnel vision, and changes in mental status such as confusion and disorientation, loss of short-term memory and some cognitive dysfunction.
Ears
Labyrinthine or inner ear DCI (the staggers) causes a combination of nausea, vomiting, vertigo, and nystagmus in addition to tinnitus and partial deafness. Labyrinthine disturbances not associated with other symptoms of DCI should be viewed as cases of barotrauma.
Lungs
Pulmonary DCI (the chokes) is characterised by (1) inspiratory burning and substernal discomfort, (2) non-productive coughing that can become paroxysmal like a coughing fit, and (3) severe respiratory distress. This occurs in about 2% of all DCI cases and can end in death. Symptoms can start up to 12 hours after a dive and persist for 12-48 hours.
CIRCULATORY SYSTEM
Hypovolaemic shock commonly is associated with other symptoms. For reasons not yet fully understood, fluid shifts from intravascular to extravascular spaces. The problems of tachycardia (rapid heart beat) and postural hypotension (dizziness when you suddenly sit or stand up) are treated by oral rehydration, if the patient is conscious or by an Intravenous infusion if unconscious. Effective treatment of DCI requires full correction of any dehydration.
Thrombi or clots may form from activation of the early phases of blood coagulation and the release of vasoactive substances from cells lining the blood vessels. The blood-bubble interface may act as a foreign surface causing this effect.
Occasionally pain originally thought to be in the shoulder joints may be due to adverse effects on the cardiac circulation mimicking heart attacks.
ABDOMINAL PAINS
These should always be treated as serious symptoms and are usually due to spinal cord damage. It is important to keep an eye on urinary output however.
PULMONARY BAROTRAUMA
Pulmonary overpressurisation, for example during a breath holding ascent, can cause large gas embolisation when rupture into the pulmonary veins allows alveolar gas to enter systemic or arterial circulation. Gas emboli can lodge in coronary, cerebral, and other systemic arterioles. These gas bubbles continue to expand as ascending pressure decreases, thus increasing the severity of clinical signs. Symptoms and signs depend on where the emboli travel. Coronary artery embolisation can lead to myocardial infarction or abnormal rhythms. Cerebral artery emboli can cause stroke or seizures.
Differentiating cerebral AGE from Type II neurological DCI is usually based upon suddenness of symptoms.
AGE symptoms typically occur within 10-20 minutes after surfacing. Multiple systems may be involved. Clinical features may occur suddenly or gradually, beginning with dizziness, headache, and profound anxiousness. More dramatic symptoms of unresponsiveness, shock, and seizures can occur quickly. Neurological symptoms vary, and death can result. Central Nervous System DCI is clinically similar to AGE; since the treatment of either requires recompression, differentiating between them is not of great importance.
PNEUMOTHORAX AND MEDIASTINAL EMPHYSEMA
These two conditions resulting from pulmonary overpressure are characterized by shortness of breath and usually follow uncontrolled or poorly controlled ascents. The former may be suspected from uneven movement of the chest and hyper-resonance on percussion of the chest wall. The shortness of breath is often relieved by assuming a sitting position andoxygen. Mediastinal emphysema can be diagnosed by the crackles felt at the root of the neck. Other than reassurance this requires no treatment. The diagnosis in both conditions must be confirmed by a hyperbaric or trauma physician and appropriate investigations done.